Klebsiella pneumoniae’s role in the “silent pandemic” of antimicrobial resistance
Main Article Content
Abstract
For decades, antibiotics have saved millions of lives, yet antimicrobial resistance is a steadily growing “silent pandemic” contributing to over 700,000 deaths per year. Antimicrobial resistance (AMR) occurs when microbes develop resistance over time so that antibiotics are no longer effective treatments.
One key player in AMR is Klebsiella pneumoniae - a highly antibiotic-resistant bacterium that is prevalent in diverse settings like hospitals and the outdoor environment. It is an especially important pathogen of newborns in developing countries. Due to its multi-drug resistance, K. pneumoniae has been classified by the World Health Organization as “critical priority” for urgent development of new antibiotics. Previous studies have analyzed the genetic makeup of K. pneumoniae strains; however, there is limited understanding of K. pneumoniae’s functional characteristics.
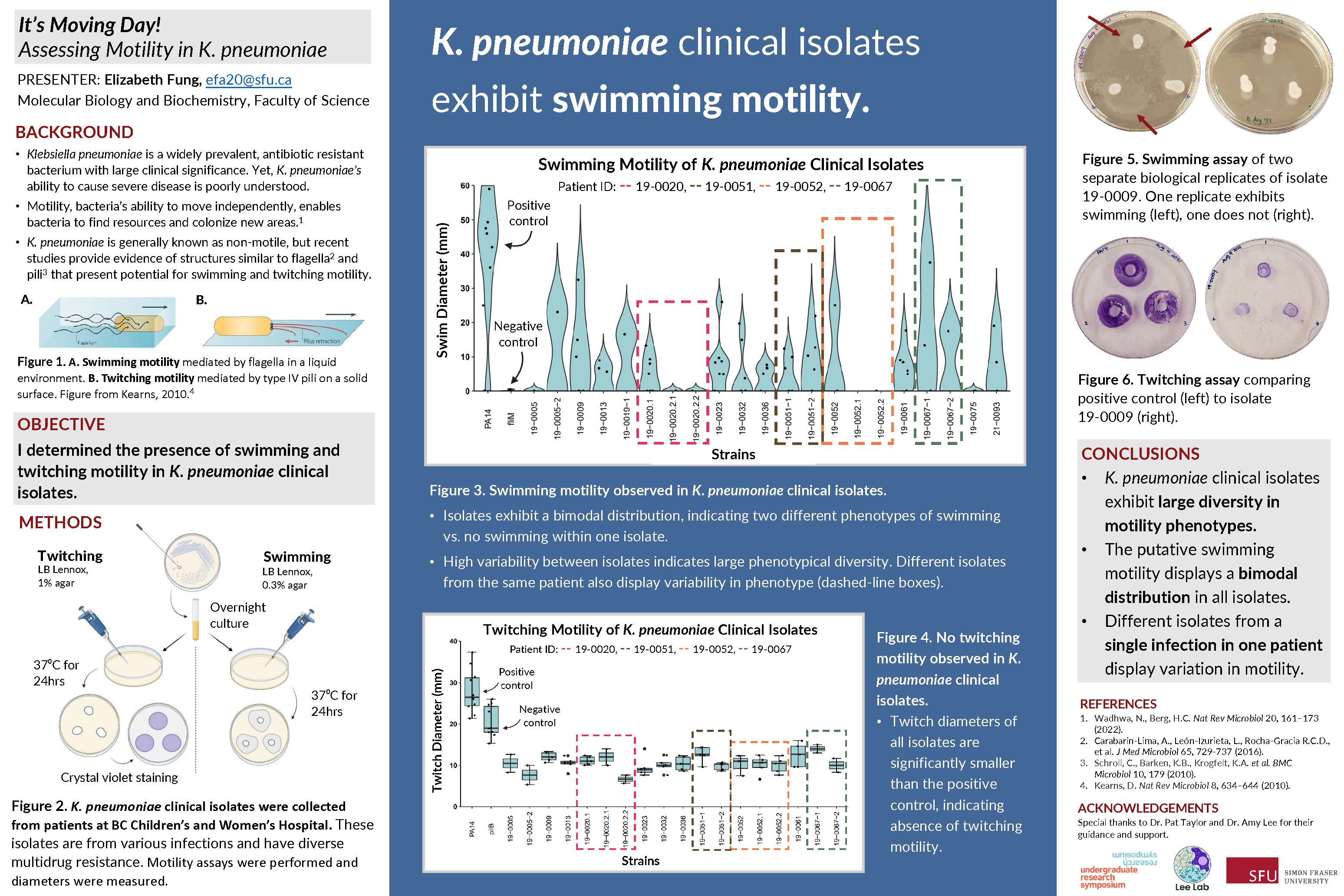
In my research, I will study a collection of K. pneumoniae clinical samples to look for traits important in colonization, resistance, and survival. Specifically, I will assess motility – bacteria’s ability to move independently to colonize new areas– and biofilm formation– multicellular aggregates of bacteria that are highly resistant to antibiotics and can easily cling to medical equipment surfaces. Both motility and biofilm formation are virulence mechanisms that allow bacteria to infect and survive in their host. By identifying trends in these characteristics between different clinical samples, I will establish phenotypic profiles of K. pneumoniae strains that can be used for further clinical and genomic analyses. Overall, my research will increase our understanding of K. pneumoniae’s functions and contribute towards stopping the “silent pandemic” of antimicrobial resistance.
Faculty Supervisor: Dr. Amy Lee, Molecular Biology and Biochemistry,, Simon Fraser University
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.